The journey to parenthood should be filled with excitement, not anxiety. While a fibroid diagnosis can feel overwhelming, most women with fibroids go on to have healthy, successful pregnancies. However, if you have fibroids, you may be concerned about conceiving and maintaining a healthy pregnancy. The risk of miscarriage due to fibroids is related to their size, type, and specific location within the uterus.
Understanding how your specific fibroids might impact your pregnancy is the first step toward peace of mind. By identifying their exact location through ultrasound, your care team can determine if fibroids might interfere with the developing pregnancy or if they are not a concern. This proactive monitoring allows you and your doctor to move from uncertainty to a clear, personalized management plan—one that prioritizes both your health and a stable environment for your growing baby.
How Do Fibroids Cause Miscarriage?
Fibroids can cause miscarriages by distorting the uterus, competing for blood flow, and minimizing the space for the fetus.
- Uterine Distortion: A large or poorly positioned fibroid can physically alter the shape of the uterus. This structural change may prevent an embryo from attaching securely to the uterine wall, making successful implantation difficult.
- Blood Flow Competition: Fibroids are living tissue that require a blood supply to grow. In some cases, they can “steal” essential nutrients and oxygen-rich blood away from the developing fetus, compromising its growth and viability.
- Space Constraints: As a pregnancy progresses, the fetus needs room to expand. Rapidly growing fibroids can increase pressure within the uterine cavity, leaving insufficient space for the pregnancy to continue safely.
In other instances, fibroids cause miscarriages by growing in a way that reduces essential blood flow to the developing fetus or by increasing internal pressure within the uterine cavity.
If you are concerned about your reproductive health, understanding the specific size and location of your fibroids is the best way to assess your risk factors.
Fibroids Impact on Early Development of an Embryo
The connection between fibroids and miscarriage often begins during the early stages of pregnancy. Even before a loss occurs, fibroids can influence the health of the pregnancy in several ways. Fibroids may restrict the physical space needed for the embryo to grow. Ultimately, whether fibroids can cause miscarriage depends on the extent to which they alter the uterine cavity and impact its function. Understanding how fibroids affect pregnancy is a vital step in managing early developmental risks.
What Types of Fibroids Are Most Likely to Increase Miscarriage Risk?
When it comes to pregnancy complications, the type of fibroid, which is determined by its location in the uterus, is the most significant factor that may increase miscarriage risk. Not all fibroids are a miscarriage risk, as their impact depends entirely on how close they are to the uterine cavity.
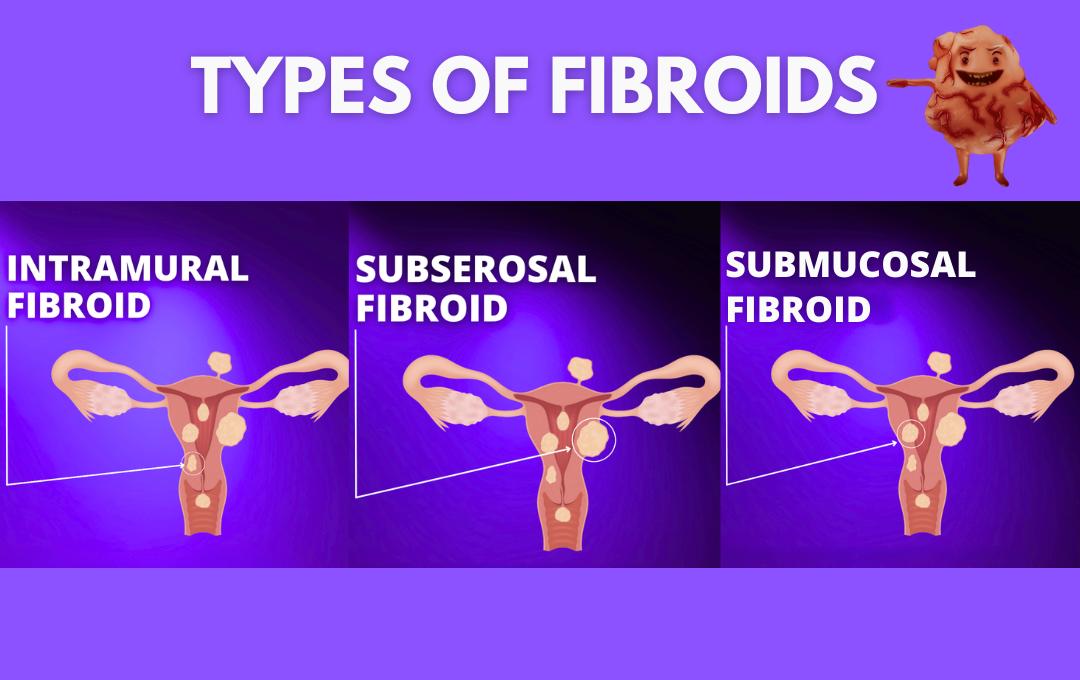
- Submucosal Fibroids: These are cited as the most problematic type regarding miscarriage risk. Because they develop just under the uterine lining and bulge directly into the cavity. They occupy the exact space where an embryo needs to implant. This can interfere with the embryo’s ability to attach or receive proper blood flow.
- Intramural Fibroids: These grow within the muscular wall of the uterus. While many go unnoticed during pregnancy, they can become a concern if they grow big enough to distort the shape of the uterine cavity or put pressure on the developing placenta.
- Subserosal Fibroids (Outside the Uterus): These grow on the outer surface of the uterus. Since they grow outward and away from the embryo, they are rarely associated with an increased risk of miscarriage.
A miscarriage due to fibroids is most likely to occur when the fibroids affect the specific area where embryo implantation or early fetal development takes place.
Because every woman’s anatomy is different, the best way to understand your personal risk is through diagnostic imaging. Identifying exactly where your fibroids are located and how they interact with the uterine lining is the most effective way to determine if they might impact your ability to carry a pregnancy to term.
What Fibroid Symptoms May Signal a Higher Risk of Miscarriage?
Fibroid symptoms that may indicate a higher risk of miscarriage include severe pelvic pain, often caused when a fibroid outgrows its blood supply, heavy vaginal bleeding, and intense cramping during the first trimester. Monitoring these symptoms is important, as they can signal complications like placental abruption or structural interference with the developing pregnancy.
Recognizing these signs is an important step in understanding how fibroid miscarriage concerns might apply to your specific health profile. Assessing these physical indicators allows for exploring the right treatment plan and pregnancy planning.
At What Trimester Can Fibroids Cause Miscarriage?
Fibroids can cause miscarriage or pregnancy complications at any trimester, though the type of risk shifts as the pregnancy progresses. The stage at which fibroids become a concern depends on their size, location, and how they interact with the developing pregnancy.
First Trimester
Fibroids are often linked to early miscarriage during the first trimester. This typically occurs when a fibroid interferes with the embryo’s ability to implant in the uterine lining. If a fibroid disrupts the area where the embryo implants or interferes with its early growth, the pregnancy may be unable to progress past the first few weeks.
Second Trimester
As a pregnancy advances, the body produces higher levels of estrogen, which can cause certain fibroids to grow rapidly. Large or poorly positioned fibroids may lead to issues in the second trimester by physically crowding the developing fetus or restricting necessary space and blood flow.
Third Trimester
In the final months of pregnancy, the primary concern shifts from pregnancy loss to delivery complications. Large fibroids can take up significant space in the lower uterus, which may prevent the baby from turning into the proper “head-down” position, increasing the likelihood of a breech birth. Additionally, fibroids located near the cervix can physically block the birth canal, which may necessitate a Cesarean section (C-section) to ensure a safe delivery for both mother and baby.
Understanding that fibroids can cause miscarriage at different stages helps in creating a proactive care plan. The care and treatment plan can vary depending on individual cases and allows you and your doctor to manage your health throughout the entire pregnancy better.
How to Avoid Miscarriage With Fibroids
Managing your health to avoid miscarriage with fibroids begins with a precise diagnosis, using advanced imaging to “map” the size and location of the fibroids, to determine if they might interfere with a pregnancy. While no method guarantees the prevention of pregnancy loss, early identification allows for a personalized care plan, such as consistent monitoring or a pre-conception myomectomy if necessary. By understanding your specific risks and tracking changes in real-time, you can make informed decisions and ensure the best possible support for a healthy pregnancy journey.
Care Plan Stages
- Preconception (Assessment): Uses imaging (ultrasound/MRI) to map fibroid “geography.” Key actions include hormonal optimization or surgical removal (myomectomy) if the uterine cavity is obstructed.
- First Trimester (Implantation): Focuses on ensuring a stable environment via frequent viability scans. Doctors monitor for rapid fibroid growth fueled by pregnancy hormones.
- Second & Third Trimesters (Growth & Comfort): Shifts to managing physical space and pain. Medical teams track for preterm labor and manage pain from fibroid tissue death using rest, hydration, and safe medications.
The Collaborative Team
Successful management relies on a multidisciplinary team of medical experts:
- OB/GYN: Oversees standard prenatal care and growth monitoring.
- Maternal-Fetal Medicine (MFM): Provides high-risk imaging and complication management.
- Fertility Specialist (REI): Optimizes the uterine environment for patients with a history of loss or those using IVF.
- Fibroid Specialist: A medical professional dedicated to diagnosing and managing uterine growths. They provide a range of treatments, from surgical removals like hysterectomy and myomectomies to non-surgical options like UFE, to alleviate symptoms such as pain and heavy bleeding.
Since the size and location of the growths dictate when they might become a contributing factor in a miscarriage, early monitoring is essential. While many women successfully carry to term, being aware of how fibroids can cause miscarriage during different months of gestation.
Fibroid Treatment Options Before Trying to Conceive
Addressing fibroids before pregnancy can relieve painful symptoms and optimize the uterine environment for conception. While many assume surgery is the only solution, modern minimally invasive and non-surgical treatments, such as uterine fibroid embolization (UFE), offer effective alternatives that preserve the uterus and involve shorter recovery times. Consulting a specialist allows you to evaluate your specific situation, especially after a loss, to determine if a procedure like UFE is the right step toward a healthier future and a successful pregnancy.
When to Talk to a Fibroid Specialist
Living with persistent pelvic pain or menstrual irregularities can be exhausting, but it is important to know that you don’t have to manage these symptoms alone. In particular, women planning for a family should be aware of the connection between reproductive health and fibroids. Research regarding fibroids and miscarriage suggests that these growths can lead to complications due to restricted blood flow or taking up space needed by the growing baby.
If you have experienced a miscarriage due to fibroids or are struggling with recurrent pregnancy loss, a specialist can help determine if the size or location of your fibroids is a contributing factor.
Beyond fertility concerns, you should schedule a consultation with a fibroid specialist if you experience the following symptoms:
- Heavy or Prolonged Bleeding: Periods that last longer than a week or require changing sanitary products every hour.
- Pelvic Pressure and Pain: A constant feeling of fullness, bloating, or sharp pain in the pelvic region.
- Urinary Urgency: Fibroids pressing against the bladder, causing frequent trips to the bathroom.
- Ongoing Fertility Struggles: Difficulty conceiving after months of trying.
Understanding your treatment options is the key to regaining control over your body and your future. Our team of highly trained fibroid specialists is dedicated to providing minimally invasive treatments that preserve the uterus and relieve painful symptoms.
Addressing Fibroids and Miscarriage Risk with Expert Guidance
While the presence of fibroids does not guarantee complications, they can affect uterine blood flow or take up space needed by the developing fetus. For women managing fibroids after miscarriage, seeking a specialized evaluation is the most effective way to improve fertility and ensure the uterus is healthy for a full-term pregnancy.
USA Fibroid Centers specializes in identifying how fibroids affect your reproductive health. Our experts offer minimally invasive treatments, such as uterine fibroid embolization (UFE), designed to shrink fibroids and alleviate symptoms without the need for major surgery. By choosing a team dedicated specifically to fibroid care, you gain access to the right diagnostics and non-surgical solutions tailored to your unique journey toward recovery and parenthood.
SCHEDULE A CONSULTATION ONLINE
Frequently Asked Questions
Could fibroids cause miscarriage?
Fibroids can cause miscarriages depending on their location. Submucosal fibroids, which grow into the uterine cavity, can interfere with embryo implantation or limit space, potentially leading to pregnancy loss.
Can fibroids come out during miscarriage?
Fibroids can not come out during a miscarriage. Fibroids are firm, muscular growths attached to the uterine wall or embedded within it. Pregnancy tissue is expelled during a miscarriage, but fibroids remain attached and require specific medical procedures for removal.
Can fibroids make you lose your pregnancy?
Fibroids can lead to pregnancy loss in some cases. Large or poorly positioned fibroids can lead to complications such as restricted fetal growth or issues with the placenta that can result in a loss.
Is It Safe To Remove Fibroids During Pregnancy?
Medical professionals generally avoid removing fibroids during pregnancy because the increased blood supply to the uterus makes surgery highly risky for both the mother and the baby. Instead, the focus is on conservative management, such as rest and pain relief, to ensure the pregnancy reaches full term safely.
Can Fibroids Cause a Premature Delivery?
Large or multiple fibroids can trigger preterm delivery by causing early contractions, particularly if the growths degenerate or prevent the uterus from stretching properly as the baby grows. Additionally, significant fibroids can place excessive pressure on the cervix, potentially leading to premature dilation or the early rupture of membranes.