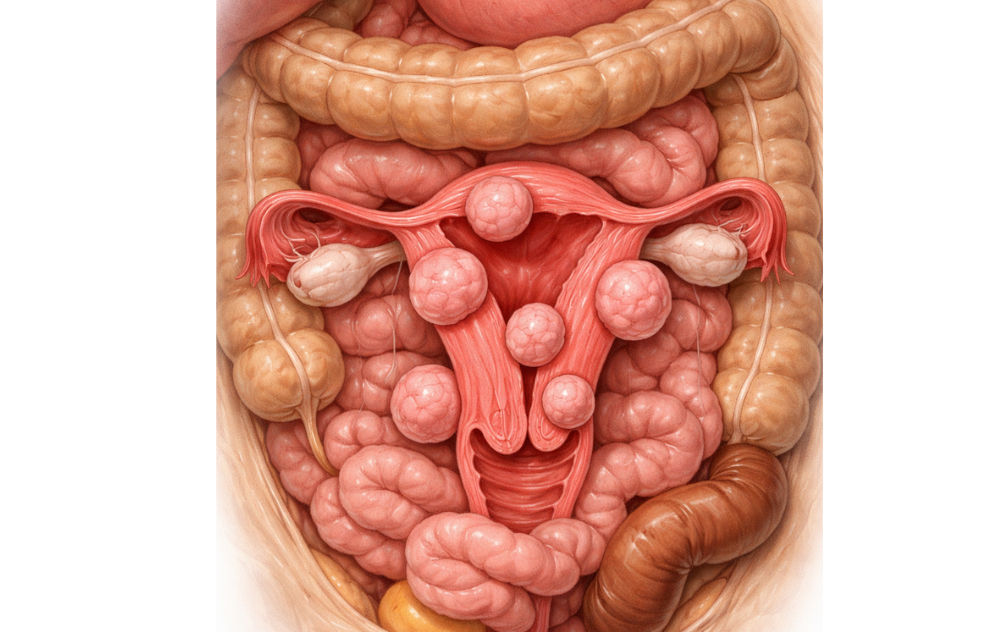
We tend to blame a slow gut or a heavy meal for constant bloating and constipation. But if you’ve tried probiotics and diet changes with no relief, the issue might not be your digestion. The reality of whether fibroids can cause digestive issues lies in your pelvic cavity, where your organs are close together. When fibroids grow, they take up significant room, especially if they are large or positioned toward the back of the uterus. Fibroids can press against the colon and rectum, creating an obstruction that disrupts regular bowel function and makes it more difficult for waste to move through your system.
If you’re feeling “backed up” or notice your bowel habits have changed, along with pelvic pressure, it’s worth considering the connection between fibroids and digestion. Understanding that these symptoms are often physical, not just dietary, is the first step toward finding actual relief.
How Uterine Fibroids Can Affect the Digestive System
Fibroids can impact your gastrointestinal health simply because of where the uterus sits in the body, making this ‘uterine issue’ a common cause of digestive discomfort. Your pelvic cavity is a tight space shared by the uterus, bladder, and bowel. When fibroids grow, they act as space-occupying masses that crowd these neighboring organs.
How fibroids affect digestion is usually through pressure, compressing the colon and rectum. This physical obstruction slows down the passage of waste, leading to several digestive problems caused by fibroids.
As these symptoms mirror common GI issues like IBS, many women don’t overlook the possibility that fibroids can affect the digestive system until an imaging test reveals the result.
Common Digestive Problems Caused by Fibroids
Common digestive problems can be caused by fibroids when they grow in size or shift position. By crowding your pelvic cavity, fibroids press on the organs that share their space. As a result of this, many women find that fibroids and digestive issues go hand-in-hand, triggering a range of gastrointestinal symptoms often mistaken for common stomach bugs or dietary sensitivities. It is important to recognize that because fibroids and gastrointestinal problems are due to physical pressure, dietary changes alone can not fix the issue at hand.
Common Digestive Symptoms
- Constipation: A fibroid pressing against the rectum or colon can physically obstruct the path, making it difficult to pass stool.
- Bloating: Unlike typical gas, this is often a constant, firm feeling of “fullness” or a visible abdominal bulge.
- Abdominal Pain: Fibroids can cause dull, persistent aches or sharp cramps that are often misidentified as gut-related.
- Acid Reflux: Large fibroids can increase internal pressure, pushing against the stomach and contributing to heartburn.
- Frequent Urination: Though urinary-related, the constant urge to go is often the most noticeable sign of a fibroid pressing on the bladder.
- Bowel Obstruction: In severe cases, extreme pressure from large fibroids can create a blockage, causing persistent nausea and inability to pass stool.
Since these symptoms are physical, they will not resolve with dietary adjustments. Fibroids that cause digestive issues are a clear sign that you should seek a professional medical evaluation to rule out underlying causes.
MAKE AN APPOINTMENT TODAY
Why Fibroid Size and Location Impact Digestion
Uterine fibroids are firm, noncancerous growths of muscle and tissue fueled by the hormones estrogen and progesterone. Because fibroids can range in size from tiny seeds to larger than a watermelon, these shifting masses often crowd the pelvic cavity—creating a variety of symptoms that can be difficult to trace back to the uterus.
How Fibroid Size Changes Things
It is very common for fibroids to increase in size over time; in fact, research suggests that most fibroids will grow significantly during a woman’s reproductive years. As a fibroid gets bigger, the uterus expands and begins to crowd the space normally reserved for your intestines.
- The “Traffic Jam”: Your intestines need to expand and contract to move food along. When a large fibroid is pressing against them, it’s like a kink in a garden hose. The path narrows, and waste moves more slowly, leading to constipation.
- The Impact of Small Fibroids: Even small fibroids can increase the overall weight and bulk of the uterus. This added weight can lead to pelvic floor dysfunction, which can indirectly affect your ability to have regular, comfortable bowel movements.
- The “Full” Feeling: Because the fibroid is taking up so much room, your stomach and intestines have less horizontal space to stretch after you eat. This is why you might feel bloated or stuffed even after a light snack.
How Fibroid Location Targets Different Areas
The symptoms change depending on exactly where the fibroid is located:
- Back of the Uterus (Posterior): The rectum sits right behind the uterus. A fibroid here pushes directly against the very end of your digestive tract. This makes it physically harder to pass stool and creates a constant feeling of pressure.
- Top of the Uterus (Fundal): If a fibroid grows upward, it starts to nudge the small intestine or the bottom of the stomach. This is usually what causes that heavy, tight feeling in your upper belly or general indigestion.
- Outside the Uterus (Subserosal): These grow outward into the abdominal cavity. If they have a stalk, they can occasionally get tangled or bump into loops of the bowel, causing sudden, sharp cramps or trapped gas.
Can Large Fibroids Cause Digestive Problems?
Large fibroids can cause digestive problems due to their location, crowding the pelvic cavity and pressing directly against the intestines. Physical pressure often leads to bloating, constipation, or a heavy feeling of fullness that lifestyle changes simply can’t fix. When digestive issues become frequent or intense, it is often a sign that fibroids are interfering with your internal organs.
Don’t just treat the symptoms. Instead, talk with a specialist to see if a non-surgical treatment is right for you.
How to Know If Fibroids Are Causing Gastrointestinal Problems
Distinguishing between a regular, everyday digestive issue and fibroids affecting digestion often comes down to pattern recognition. Identifying if fibroids may be the reason behind the digestive problems involves a group of symptoms:
- Full Gut: Feeling increased pressure or a “full” sensation in the gut that worsens when you lie down or during certain movements.
- Bloating/Constipation: If your digestive issues—such as bloating or constipation—consistently flare up or worsen in tandem with your menstrual cycle.
- Lower Pelvic Pressure: Experiencing a frequent urge to go or a feeling of “incomplete” evacuation that feels more like external pressure than internal cramping.
If you notice these patterns, scheduling a pelvic exam with a fibroid specialist to see if fibroids are affecting your digestion may be helpful.
When Digestive Problems May Signal Something More Than Fibroids
Even though fibroids can often cause pelvic or abdominal pressure, persistent or severe gastrointestinal symptoms should always be evaluated to rule out other underlying causes. It is important to remember that having fibroids does not rule out the possibility of a coexisting digestive condition. Immediate medical care is required if you experience any of the following symptoms:
- Blood in the stool or unexplained weight loss.
- Persistent vomiting or severe, worsening abdominal pain.
- Fever accompanying digestive distress.
- New, progressive constipation, especially if paired with significant abdominal swelling.
What An Accurate Diagnosis Looks Like
An accurate diagnosis is required to ensure you aren’t treating the wrong condition. Since symptoms like bloating or pelvic pressure can overlap with other issues, a fibroid specialist should rule out or confirm the presence of fibroids. This is particularly important because fibroids and gastrointestinal problems are often interconnected.
Confirming whether fibroids can cause digestive issues allows for a targeted treatment plan rather than assuming symptoms are strictly hormonal. To reach a decision for suitable treatment, a proper diagnosis, often involving an ultrasound or physical exam, is necessary to differentiate between digestive problems and fibroids.
Assessment for Fibroids
- Physical (Pelvic) Exam: A provider manually feels the abdomen and pelvis to check for an enlarged, irregular, or firm uterus, which is a classic indicator of fibroids.
- Transvaginal Ultrasound: This is the gold-standard initial imaging test. It provides high-resolution images of the uterus, allowing the clinician to identify the number, size, and location of fibroids.
- MRI (Magnetic Resonance Imaging): If an ultrasound is inconclusive or the fibroids are particularly large/numerous, an MRI offers a more detailed “map” of the pelvic anatomy.
Assessment for GI Problems
If the physical exam and ultrasound clear the uterus of the presence of fibroids, the focus shifts to the digestive system.
- Symptom Mapping: Doctors differentiate by looking for symptoms that point to the gut rather than the reproductive system, such as changes in bowel habits(diarrhea/constipation), blood in the stool, or unexplained weight loss.
- Endoscopy: To rule out structural issues like polyps, inflammatory bowel disease (IBD), or diverticulitis, a gastroenterologist may use a camera to examine the lining of the digestive tract.
Treating Uterine Fibroids’ Digestive Issues
Treating fibroid-related digestive issues requires relieving pressure on the bowel. While surgeries like hysterectomy or myomectomy are common, they involve significant recovery and risks, including potential nerve disruption, adhesions, or rare bowel injury.
A safer, minimally invasive alternative is uterine fibroid embolization (UFE). UFE blocks the blood supply to the fibroids, causing them to shrink and die. This effectively reduces pressure on digestive organs without the need for major surgery. If you experience severe post-surgical pain or vomiting, seek medical attention immediately.
Benefits of UFE
- Surgery Risks: Recovery can involve “shifting” organs or adhesions that prolong digestive discomfort.
- UFE Advantage: Shrinks the fibroids naturally to clear the “traffic jam” in your abdomen.
- Safety: UFE avoids the surgical risks of bowel injury or permanent nerve disruption.
Managing Digestive Symptoms
If you are experiencing persistent digestive issues and discomfort, it is important to stop managing the symptoms. While hormonal shifts are common, investigating whether your symptoms have a physical cause can be beneficial.
Can uterine fibroids cause digestive problems? Many women are surprised to find that the answer is yes. The link between fibroids and digestive issues is clear when growths become large enough to press on surrounding organs. If you are experiencing chronic bloating, bowel pressure, or a frequent sense of fullness, it is time to consult your doctor.
At USA Fibroid Centers, our specialists provide uterine fibroid embolization (UFE), a minimally invasive alternative designed to deliver lasting relief without the risks or lengthy recovery of major surgery. We understand how symptoms like chronic constipation and heavy cycles can disrupt your life; our goal is to ensure you receive the right care for lasting relief.
By targeting fibroids without surgery, UFE addresses the physical pressure on your digestive tract and restores your quality of life. Schedule your consultation at a nearby clinic today.
SCHEDULE A CONSULTATION ONLINE NOW
Frequently Asked Questions
Can fibroids cause IBS-like symptoms?
Fibroids, especially large ones, can cause irritable bowel syndrome (IBS) like symptoms. When they press on the bowel or rectum, uterine fibroids can cause symptoms such as bloating, constipation, or rectal pressure.
Can fibroids make your stomach upset?
Fibroids do not directly cause stomach upset (like nausea or indigestion), but they can create physical discomfort in the pelvic and abdominal area. The pressure they exert on neighboring organs can lead to a sensation of fullness or abdominal bloating.
Can probiotics shrink fibroids?
There is no scientific evidence that probiotics can shrink existing fibroids. While probiotics support gut health and may help manage digestive symptoms, they cannot reduce the size of fibroid growths.