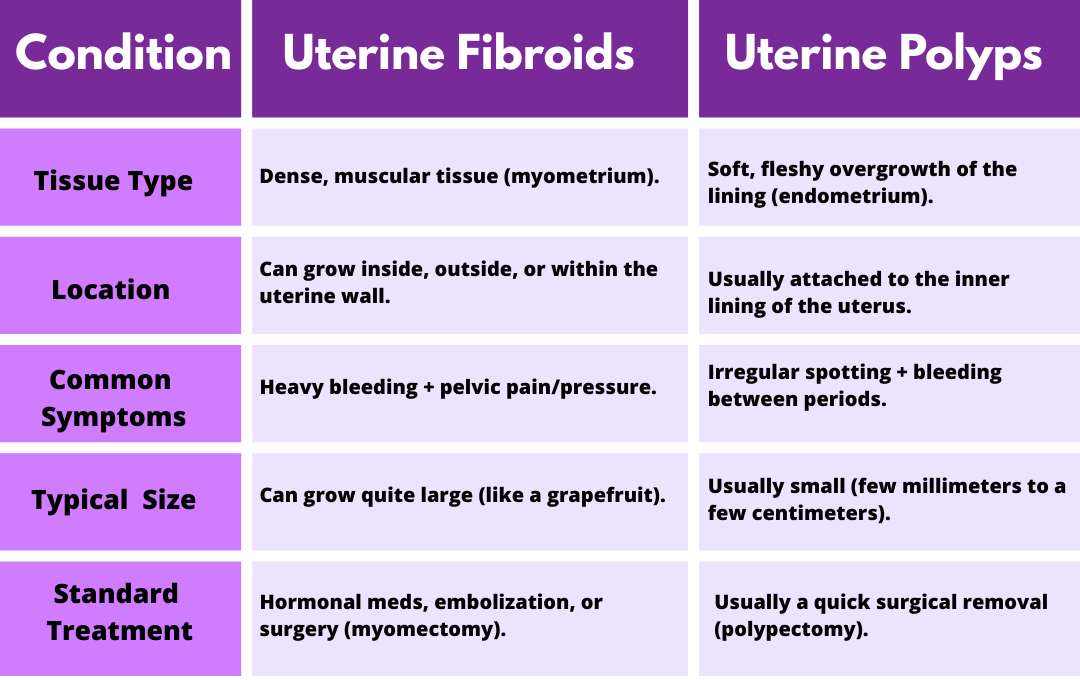
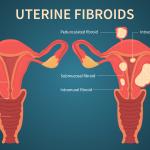
When it comes to uterine health, polyps and fibroids are the two most common reasons for irregular menstrual bleeding. However, they aren’t interchangeable. Polyps are soft overgrowths of the uterine lining, primarily responsible for irregular spotting. In contrast, fibroids are dense muscle masses that often lead to persistent pelvic pressure and bloating.
Are Polyps More Dangerous Than Fibroids?
While generally benign, uterine polyps carry a slightly higher malignancy risk (1% to 6%) than fibroids, particularly depending on menopausal status. This difference exists because polyps are more prone to developing precancerous cells than the muscle tissue that forms fibroids.
Polyps and fibroids symptoms often overlap so closely that it’s nearly impossible to tell them apart without medical evaluation. To get a better handle on what’s happening, we need to look at how these growths differ in composition, how they impact your body, and the specific ways they are diagnosed and treated.
Understanding The Difference Between Uterine Fibroids and Polyps
When you’re dealing with heavy periods or pelvic pressure, it’s easy to lump all “growths” into the same category. The difference between polyps and fibroids can be significant, as they originate from different tissue types and often require different approaches to care.
While both are typically noncancerous, the main distinction between polyps and fibroids often comes down to texture and size. Fibroids are like firm rubber balls that can change the shape of your uterus, whereas polyps are more like skin tags; small, fragile, and prone to causing breakthrough bleeding.
Fibroids vs. Polyps Symptoms
When dealing with reproductive health, it can be difficult to distinguish between fibroids vs. polyps because their symptoms often overlap. However, the way these growths affect your body typically follows different patterns. While both can cause heavy menstrual cycles, understanding the specific nuances can help you identify what you are experiencing.
While both conditions impact the reproductive system, the patterns of fibroids vs. polyps differ significantly. The most common symptoms of uterine polyps involve irregular spotting or unpredictable breakthrough bleeding, whereas fibroid symptoms are more notorious for causing consistently heavy, prolonged periods with large clots. Furthermore, while fibroids often create a distinct sense of pelvic pressure that can lead to frequent urination or constipation, polyps are typically much smaller and rarely impact the bladder or bowel. Even the associated discomfort varies: fibroid pain often manifests as a dull, heavy ache during menstruation, while a symptom of a polyp in the uterus is more likely to be mild, random cramping throughout the month.
Bleeding Differences: Spotting vs. Heavy Flow
The most distinct way to tell the difference between uterine polyps vs. fibroids is often found in your menstrual calendar. While both can disrupt your life, the “style” of bleeding usually differs. Uterine polyps are growths in the endometrial lining, which can cause mid-cycle spotting or unpredictable bleeding between periods.
On the other hand, the main difference between a fibroid vs. polyp is volume. Fibroids, especially those that bulge into the uterine cavity (submucosal) or sit within the muscular wall (intramural), increase the surface area of the uterine lining and prevent the uterus from contracting efficiently. This typically results in flooding or heavy, prolonged periods that last well beyond the standard seven days. Essentially, while polyps can be considered the masters of irregular timing, fibroids are masters of excessive flow.
Pain, Pressure, and “Bulk” Symptoms
When comparing uterine fibroids or polyps, the main difference is “bulk.” Fibroids can grow large enough to cause persistent pelvic pressure and secondary symptoms like urinary frequency due to bladder compression.
In contrast, polyps and fibroids differ in size; they stay small and rarely cause that heavy, bloated feeling.
What Causes Polyps and Fibroids?
While researchers are still studying the exact reasons why uterine fibroids or polyps develop, the main driver for both is often hormonal fluctuations. Specifically, an overgrowth of cells is frequently linked to estrogen levels. When estrogen increases, it can cause these growths to develop or enlarge; when levels drop, they may shrink.
While they share a hormonal connection, the risk factors for a fibroid vs. polyp can vary slightly:
- Hormones: High levels of estrogen and progesterone are primary causes of fibroids and are also linked to the development of polyps.
- Age and Weight: Both polyps and fibroids are more common as you approach menopause or if you have a higher body weight, which can increase estrogen production.
- Health History: High blood pressure or a family history of these growths can also play a role.
It is important to remember that polyps and fibroids are very common, non-cancerous conditions. Most of the time, they are simply a result of the body’s natural chemistry and can be managed effectively with the right care and, in some cases, the right treatment.
Can You Have Fibroids and Polyps at the Same Time?
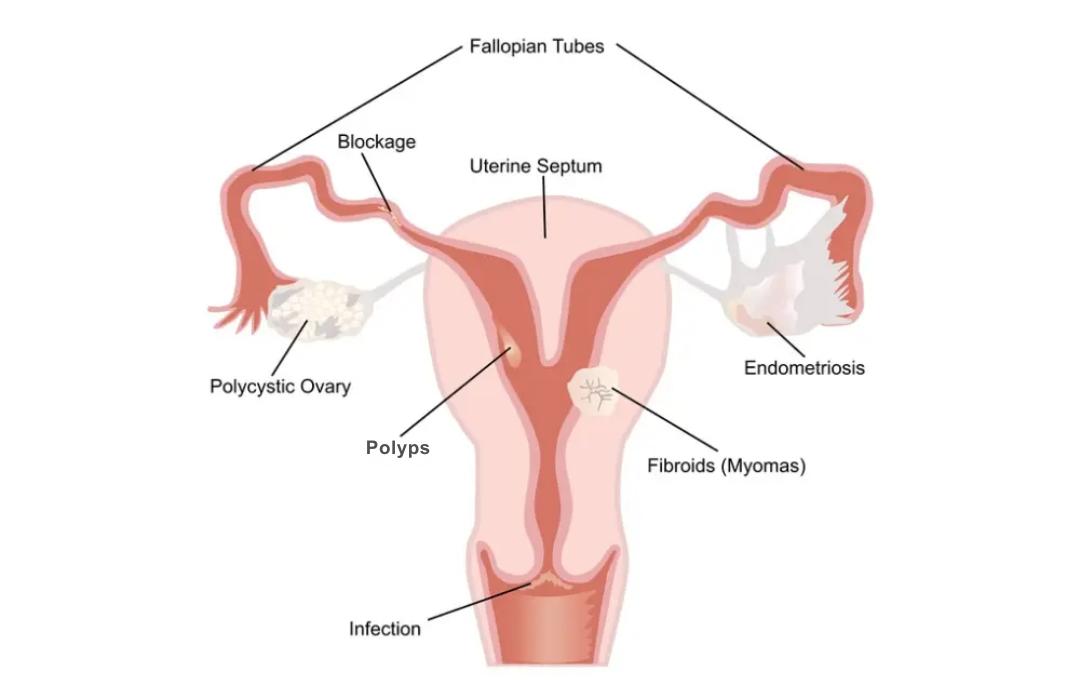
It is quite possible to have both polyps and fibroids simultaneously. Since they grow in different parts of the uterus, polyps in the lining and fibroids in the muscle, they don’t “compete” for space, and having one doesn’t prevent the other from developing.
When you have both uterine fibroids and polyps, your symptoms might be a confusing mix of heavy flow and random spotting. If your cycles don’t entirely match the description of just one condition, a professional evaluation is required. Determining if you have both is the only way to ensure your treatment plan addresses every source of your discomfort.
What Happens if you Have Fibroids vs Polyps?
Once you understand the difference between these two growths, the next question is how they impact your treatment path. While both can cause life-disrupting symptoms, they are managed very differently based on their composition.
- For Uterine Polyps: Polyps are growths in the uterine lining (endometrium), and they are typically removed through a simple, quick procedure called a hysteroscopic polypectomy.
- For Uterine Fibroids: Because fibroids are dense, muscular masses that often require a more robust approach, especially if they are causing symptoms like pelvic pressure or bladder compression. There are several ways to address the muscle tissue, ranging from hormone therapy, surgical removal (myomectomy), to uterine fibroid embolization (UFE), which shrinks the fibroids and leaves the uterus intact.
Can You Have UFE for Fibroids if You Also Have Polyps?
If you have both uterine fibroids and polyps, you may wonder whether they can be treated at the same time. The answer is yes, but because polyps and fibroids are made of different tissues, they often require a coordinated care plan. Uterine Fibroid Embolization (UFE) is a breakthrough, non-surgical procedure designed to shrink fibroids by cutting off their blood supply.
Treating both ensures you aren’t just masking the symptoms, but actually addressing the entire cause of your discomfort.
How to Check for Fibroids or Polyps
If you are experiencing symptoms, the first step in checking for fibroids or polyps is a consultation with a specialist. Since uterine polyps vs. fibroids share similar traits, doctors use specific imaging to see what is happening inside the uterus.
Here is what you need to know if you have both:
- The Diagnostic process :
- Before undergoing UFE, imaging such as an ultrasound or MRI helps your doctor distinguish between the muscular tissue of a fibroid and the softer tissue of a polyp.
- Because polyps are made of soft, mucosal tissue (the same material as your uterine lining), they often blend in on a traditional “dry” ultrasound. If a polyp is suspected, but the standard ultrasound is inconclusive, they will often perform a Saline Infusion Sonogram (SIS).
- The “Two-Step” Approach:
- Doctors often recommend removing the polyp first. Once the polyp is cleared, UFE can be performed to address the larger, more painful fibroids.
The fibroid experts at USA Fibroid Centers use advanced diagnostic imaging to ensure an accurate diagnosis and pinpoint the exact cause of your discomfort. Schedule a consultation online with a specialist and verify your insurance coverage in real-time.
MEET A FIBROID SPECIALIST FOR A DIAGNOSIS
Treatment Options for Fibroids vs Polyps
Choosing the right treatment for fibroids vs. polyps depends on several factors, including the severity of your symptoms, the size and location of the growths, and your future fertility goals. Since a fibroid vs. polyp can impact your health differently, treatment should address your specific bleeding patterns and pain levels. Whether you are dealing with uterine polyps vs. fibroids, the goal is to determine the most effective, least invasive method possible to restore your quality of life
Treating Uterine Polyps
Treatment for polyps often depends on whether you are experiencing the symptoms of a polyp in the uterus, such as irregular spotting or infertility. In some cases, especially for small, asymptomatic polyps, a doctor may suggest “watchful waiting” to see if they resolve on their own. However, if the symptoms of uterine polyps become disruptive or if there are concerns about cell changes, a polypectomy is usually recommended.
Treating Uterine Fibroids
When comparing treatments for fibroids vs. polyps, fibroid management often involves more variety due to their potentially larger size. For uterine fibroids or polyps, medication may be used to manage heavy flow, but it typically does not make the growths disappear.
For those seeking lasting relief, there are several uterine fibroid treatment options available. While surgical options like a hysterectomy or myomectomy exist, many women now choose more advanced minimally invasive procedures like uterine fibroid embolization (UFE). UFE is a non-surgical alternative that shrinks fibroids by cutting off their blood supply, allowing patients to avoid major surgery while effectively ending heavy bleeding and pelvic pressure. Benefits include a quicker recovery time with no hospital stay and less risk than more invasive surgical fibroid removal.
Getting Answers and the Right Treatment with USA Fibroid Centers
If you are struggling with irregular bleeding and pelvic pain, consulting a specialist who can distinguish whether your symptoms stem from fibroids vs. polyps is the first step toward relief.
Managing uterine polyps vs. fibroids requires a precise, personalized approach to care. If fibroids are the primary source of your pain, USA Fibroid Centers offers uterine fibroid embolization (UFE) for lasting symptom relief. This non-surgical, outpatient treatment is designed to shrink fibroids and stop heavy bleeding without the scars, risks, or long recovery times associated with invasive surgery. Don’t ignore persistent changes in your cycle and schedule an evaluation to learn more.
Frequently Asked Questions (FAQs)
Are polyps and fibroids the same?
Polyps and fibroids are not the same. Fibroids are made of muscle from the uterine wall, while polyps are made of the uterine lining (endometrium).
What is worse, uterine fibroids or polyps?
Neither uterine fibroids or polyps are necessarily “worse,” but they cause different problems. Polyps often cause random spotting and can affect fertility. Fibroids can grow much larger, causing heavy bleeding and painful pelvic pressure.
Can a fibroid be mistaken for a polyp on ultrasound?
Fibroids can be mistaken for a polyp, as both fibroids and polyps can look similar on a standard ultrasound scan.
How do I know if I have fibroids or polyps?
Imaging tests are needed to know if you have fibroids or polyps. Generally, heavy periods and pressure point to fibroids, while light spotting between periods points to polyps.