Did you know that over 38 million Americans have diabetes? With millions more living with prediabetes, managing blood sugar is a vital part of overall health especially for women of reproductive age.
While diabetes, irregular periods, and uterine fibroids are common conditions, emerging evidence suggests they may be more interconnected than we think. Understanding this relationship is key to achieving a complete diagnosis and effective treatment.
How Diabetes May Affect Uterine Health
Diabetes is a chronic condition that impairs your body’s ability to process sugar (glucose). When blood sugar levels are chronically high, it can damage blood vessels and nerves throughout the body, including the reproductive system. This damage and the related metabolic changes can contribute to menstrual and uterine issues. Here are the three core ways these conditions may be linked:
- Hormonal Imbalances: Diabetes can disrupt the delicate balance of reproductive hormones. High blood sugar levels may increase the production of androgens (male hormones), which are known to contribute to irregular periods and an increased risk or growth of fibroids.
- Insulin Resistance: Insulin resistance occurs when the body’s cells become less responsive to insulin. This condition is a hallmark of Type 2 diabetes and Polycystic Ovary Syndrome (PCOS). This metabolic dysfunction is also associated with an increased risk and growth of uterine fibroids.
- Chronic Inflammation: Chronic, low-grade inflammation is a key factor in the development of many chronic diseases, including Type 2 diabetes and heart disease. Research suggests that chronic inflammation may also play a role in creating the environment that encourages the development and growth of fibroids.
Can Fibroids Affect Blood Sugar Levels?
Fibroids don’t directly raise your blood sugar on their own. However, the things that cause fibroids to grow are often the same things that cause blood sugar problems. Specifically, conditions like insulin resistance (which can lead to pre-diabetes or Type 2 diabetes) create an environment that feeds fibroids.
When your body becomes resistant to insulin, it produces more insulin. This extra insulin, along with certain growth factors, acts like a fertilizer for fibroid cells, making them more likely to grow. Additionally, high insulin levels can disrupt your hormones, leading to an increase in estrogen levels in the body, which is the primary fuel for fibroids.
So, while fibroids may not be directly changing your blood sugar, the root cause of high blood sugar (insulin resistance) can be a major reason for their development.
Could Your Diabetes Be Masking Fibroid Symptoms?
Conditions like diabetes, prediabetes, and PCOS can cause symptoms that mimic those of other gynecological issues. This can sometimes mask or delay the diagnosis of underlying problems like uterine fibroids.
If you have diabetes, irregular periods, or frequent urination may simply be a sign of poorly controlled blood sugar. However, these are also hallmark symptoms of uterine fibroids, which are non-cancerous growths found in the uterus that affect up to 80% of women by age 50.
It is important to discuss your full range of symptoms with your doctor. They can determine whether you need a simple blood sugar adjustment or additional tests, such as a pelvic ultrasound, to screen for fibroids or other conditions like endometriosis or adenomyosis.
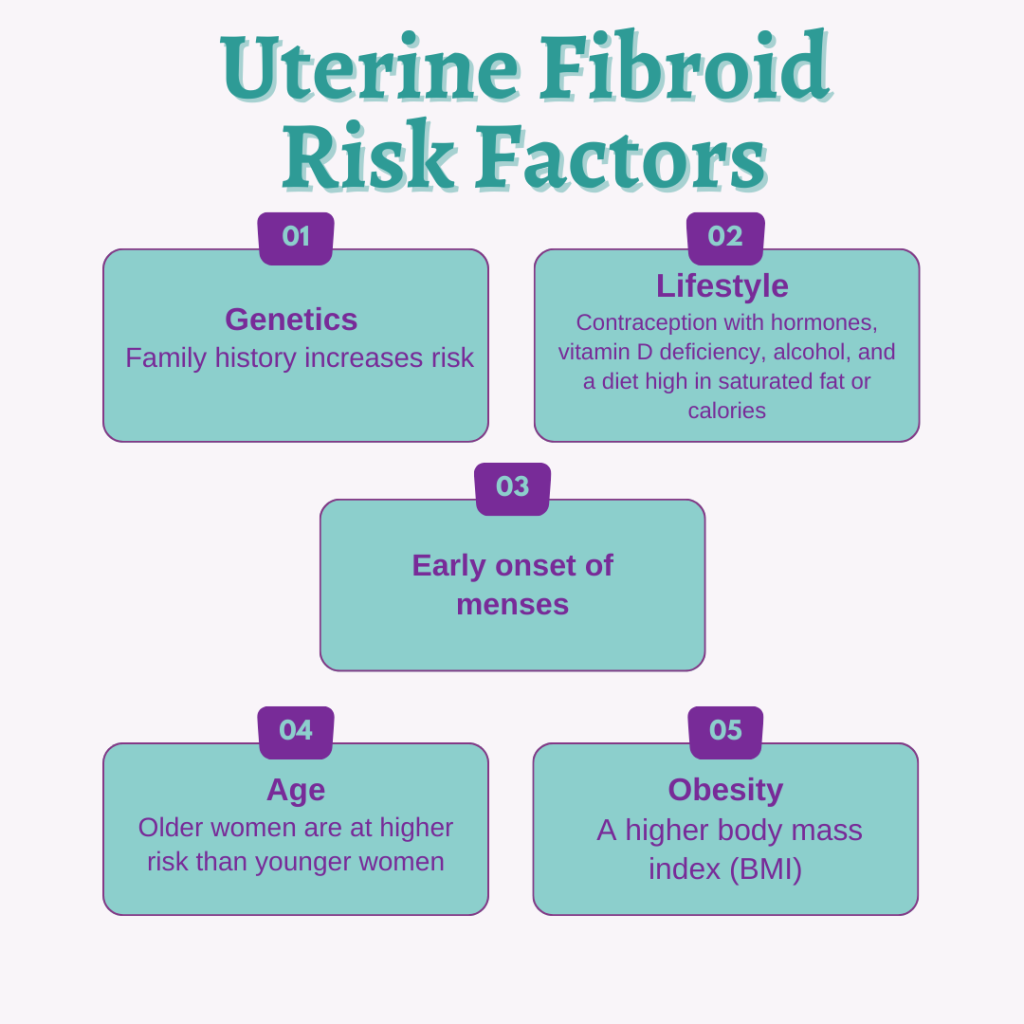
Many of the same risk factors for fibroids are similar to those associated with Type 2 diabetes.
If you are at risk for diabetes, it’s important for you to be proactive about your health. Did you know that Type 2 diabetes can be prevented or delayed with lifestyle changes, such as losing weight and being more physically active?
Diabetes or pre-diabetes isn’t the only condition that can cause your irregular periods, urinary urgency, or fatigue. Uterine fibroids often cause these symptoms.
Could Diabetes Be Affecting Your Period?
Diabetes may affect your menstrual cycle and overall uterine health. During menstruation, the fluctuation of various hormones often causes a rise in blood-sugar levels. This can lead to hyperglycemia if not managed and monitored properly. Hyperglycemia is very serious as it can cause damage to the blood vessels when left untreated.
Changes in your hormone levels before and during your period can often make blood sugar levels difficult to predict. You may also have longer or heavier periods, and food cravings can make managing diabetes harder. You should track this pattern to notice any changes over time.
Fibroid Symptoms
Because fibroid symptoms can be similar to those of other female health conditions, we recommend discussing your symptoms with your doctor. If you are diagnosed with uterine fibroids, it may be good to visit a fibroid specialist and learn about your full range of treatment options.
Diabetes and The Menstrual Cycle: When to Worry
Monitoring Your Cycle and Blood Sugar
If you have diabetes, managing your blood sugar becomes a dynamic process that is affected by your menstrual cycle:
- Hormone Fluctuations: The rise and fall of hormones before and during your period can cause your blood sugar levels to become unpredictable and harder to manage.
- Hyperglycemia Risk: Unmonitored blood sugar spikes (hyperglycemia) are serious and can damage blood vessels. Women with diabetes must monitor closely and adjust insulin as needed during their cycle.
- Cravings: Intense cravings for carbs, fats, or sweets before or during your period are common for all women (diabetic or not), often due to the body attempting to boost low serotonin levels. If you have diabetes, it’s vital to indulge in moderation to prevent dangerous blood sugar spikes.
If you have been diagnosed with diabetes, it means that you should monitor your blood sugar levels more closely. This is to ensure you’re getting the proper amount of insulin and that you are not at risk of becoming hyperglycemic. For women that are not diabetic, their blood-glucose levels can also fluctuate, but since their pancreas is relatively healthy, they are able to produce insulin to control blood sugar naturally and involuntarily.
Maintain a log that tracks both your menstrual cycle dates and your blood glucose readings. This can reveal patterns and help your care team optimize your treatment plan.
Diabetes and Perimenopause
For many women, navigating uterine fibroids and diabetes simultaneously means dealing with a tricky overlap of symptoms and treatment challenges. It’s not just about managing two separate conditions; it’s about understanding their complex, interwoven relationship, especially during the hormonal shifts of perimenopause.
Worsened Symptoms and Masked Diagnosis
When diabetes and fibroids coexist, they can create a frustrating cycle that intensifies symptoms and makes diagnosis difficult.
Amplified Symptoms
Both perimenopause and diabetes can individually cause heavy, irregular periods. When a woman has fibroids plus hormonal changes plus diabetes, the symptoms can be much more severe:
- Heavier and Longer Periods: Fibroids are notorious for causing excessive bleeding. Add in the hormonal fluctuations of perimenopause and the potential for irregular bleeding from diabetes, and you can experience debilitating blood loss and anemia-related fatigue.
- Increased Pain and Fatigue: The combination can lead to more severe pelvic pain and chronic fatigue, making it harder to distinguish the source of the discomfort.
Delayed Diagnosis (The Masking Effect)
The shared symptoms of both conditions can easily mask the presence of fibroids. For example, a healthcare provider might initially attribute heavy periods, frequent urination, or fatigue solely to diabetes or perimenopause. This overlap can lead to a delay in the proper diagnosis of fibroids, postponing necessary treatment. A key part of care is figuring out: is the heavy bleeding due to hormonal shifts, fibroids, or a diabetes-related issue?
The Hormone Connection and Treatment Challenges
Hormones, particularly estrogen, progesterone, and insulin, are central to understanding the link between these two conditions, which creates real challenges for treatment planning.
The Role of Insulin and Perimenopause
While estrogen and progesterone fuel fibroid growth (which is why fibroids often shrink after menopause), the hormone insulin also plays a significant role:
- Insulin Resistance: A common feature of Type 2 diabetes, insulin resistance can increase certain growth factors in the body. These growth factors may actively promote the growth of fibroids.
- Perimenopause Complications: During the years leading up to menopause (perimenopause), estrogen and progesterone levels fluctuate wildly. This instability can cause fibroids to grow or shrink unpredictably, leading to the worst symptoms before they eventually shrink post-menopause.
Complicating Treatment
Managing both conditions requires careful coordination because treatments for one can directly affect the other:
- Fibroid Treatment and Blood Sugar: Some common hormonal treatments for fibroids can negatively impact blood sugar levels, making diabetes management much harder.
- Diabetes Medications and Fibroids: Conversely, some diabetes medications, such as metformin, have been linked in some studies to a reduced incidence or growth of fibroids.
- Hormone Replacement Therapy (HRT): For a woman with a history of fibroids, taking HRT after menopause could reintroduce high hormone levels and cause the fibroids to grow again, bringing back symptoms.
For a woman in her mid-40s dealing with both conditions, the most important step is careful coordination with a doctor to choose a fibroid treatment plan that won’t disrupt blood sugar control, while also monitoring how diabetes medications might influence fibroid growth.
Why Listening to Your Body Is Key
Diabetes could potentially mask underlying conditions like uterine fibroids, adenomyosis, PCOS, or endometriosis. Diabetes can lead to heavier or longer periods, urinary urgency, period irregularity, or fatigue. These are also symptoms commonly associated with uterine fibroids. It’s important to write down your symptoms, so you can discuss them with your doctor. They will be able to determine if additional tests, like an ultrasound or pelvic examination, are necessary.
Should You Be Screened for Fibroids?
You may experience some symptoms of uterine fibroids that prompt you to talk to your doctor. Some of the symptoms of fibroids include:
- Heavy bleeding
- Prolonged periods
- Irregular periods
- Severe cramping
If you you are also at risk or have been diagnosed with diabetes, an accurate diagnosis is important. At our fibroid centers, we exclusively offer a non-surgical, outpatient treatment known as uterine fibroid embolization (UFE) to treat uterine fibroid symptoms. UFE utilizes a minimally-invasive technique to interrupt the blood flow to the fibroids, which will cause the fibroids to shrink. Once the fibroid does not get the oxygen and nutrients it needs to survive, it will naturally die off. This often leads to diminished symptoms.
Find Fibroid Relief at USA Fibroid Centers
With more than 40 treatment facilities across the nation, we are currently the largest network of fibroid centers in the United States. Our leading interventional radiologists utilize the most advanced technology to treat uterine fibroids. If you are experiencing heavy, irregular periods, urinary urgency, fatigue from anemia, pelvic pain or cramping, call us at 855.615.2555 to find out how we can help begin your recovery.
Don’t feel like calling? You can also schedule an appointment with us online by clicking the button below.